Infertility can be a hard thing to talk about and really understand if you have not tried it on your own body. Read about dr. Anne Judge's experience with infertility and all of the emotions attached to the process.
As a past infertility patient I often felt like infertility was a test where I had studied for the wrong topic. I knew all about birth control, healthy living, and what to expect when I was expecting. I even did a preconception visit with my somewhat bemused obstetrician before dramatically putting away my birth control pills. I did not expect to feel like a failure at one of the strongest forces of nature—reproduction. And during our years of treatment I felt I had some outlet for my sadness. Friends and relatives had a (limited) bucket of sympathy and would listen supportively…before trying to cheer me up with suggestions about relaxing, taking a vacation, or considering adoption. But I was surprised with how angry I felt about the unfair nature of it all. About how I could do everything “right” and still not get pregnant, at the same time that Teen Moms was a hit show on TV. I also had many questions, so many that my role as a patient lead me to shift careers and become a care provider at an infertility clinic.
I hope this article can explain to you the “how and why” of what goes on during infertility treatment. But more importantly, I hope to remind you that however you are feeling about it is ok.
Fertility testing and diagnosis at the clinic
The first step is always going to be fertility testing and diagnosis. Sometimes this can be frustrating as you may feel like every month is a wasted opportunity. Yet taking the time to thoroughly evaluate all the factors that go into fertility allows a clinic to make the best recommendation for treatment. Because all the milestones of pregnancy (conception, implantation, embryo growth and development) happen within the woman’s body, the focus of most fertility testing also involves the woman’s body.
Other articles explain the rationale and logistics of testing, but every diagnosis has its own challenges. People being told the only option is assisted technologies like IVF often feel the loss of not hoping for a surprise spontaneous pregnancy. One patient who had to have both her fallopian tubes removed told me she felt like she had “been fixed,” just like her cat. Those facing “unexplained infertility” mention the stress of uncertainty, and how it is difficult to undergo the discomforts and expense of fertility treatment without a clear rationale.
Regardless of the rationale and treatment plan, once a plan is made the next visits typically follow a similar pattern at the clinic. Let’s now explain the mysteries of why you pay money to come see us and be poked and prodded.
Putting sperm into your body (ever) leads to pregnancy…
Understanding what is happening inside the body involves information from the ovaries, uterus, and brain. While school sex education gives the impression that putting sperm into your body (ever) can lead to pregnancy, there are actually fairly limited windows for conception.
Humans are in the minority among mammals by having what is known as concealed ovulation. Many other species are both aware of their fertile window and advertise it with physical changes, odors, and behaviors to indicate the time for intercourse is now!
Historically, it is only recently that women been able to more reliably understand when they are ovulating by temperature trackers, apps, or urine ovulation kits have. Here in the clinic we use ultrasound and blood hormone tests to better understand and encourage the development of eggs and ovulation.
Ultrasound to access fertility
First let’s talk about ultrasound. Many women are intimidated by the idea of a transvaginal ultrasound (TVUS). I reassure women that the probe only enters the vagina a few inches, and that while they will feel some initial pressure from the probe, the rest of the exam should not be painful. The reason we use TVUS is that it allows us to put a ‘spotlight’ right against the uterus and ovaries to better ‘see’ with the sound waves of ultrasound.
Abdominal ultrasound provides a wide view of the pelvis, but with less detail. For abdominal ultrasound having a full bladder is useful for the best images, but for a TVUS we actually will see best with an empty bladder. Having a good view of the pelvis lets us examine the uterus for abnormalities (like fibroids or polyps). It also allows us to assess the ovaries for cysts or signs of endometriosis, and get an idea of egg supply. Although the egg is gigantic in size compared to sperm, it is still too small to see with ultrasound.
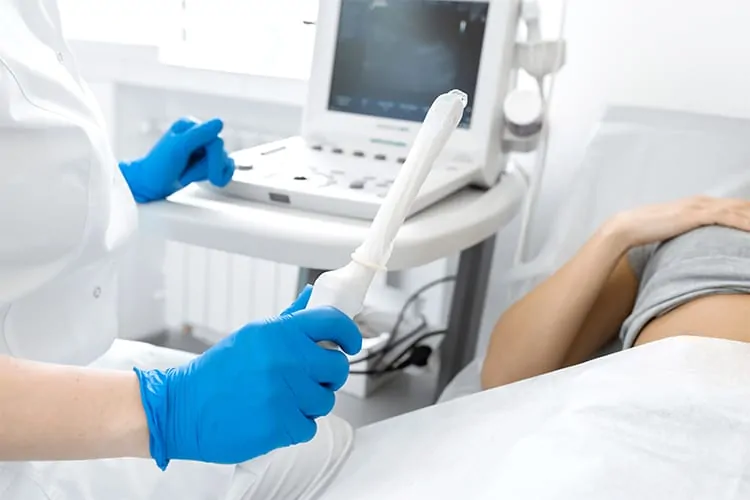
What we see on ultrasound are small dark circles of fluid called “follicles” that each contain a microscopic egg, and counting how many follicles we see on each ovary tells us about overall egg supply.
Follicle assessment
In an ovulatory cycle without fertility medications, typically only one egg grows. As the egg matures, the cells on the ovary surrounding the egg put out more fluid. So while an ultrasound done in the first week of your period may show several small follicles (the “egg allowance” for that month), by mid-cycle we hope to see one large circle of fluid that we call the “dominant follicle”, meaning the egg inside is maturing and preparing for ovulation.
By measuring the size of the growing circle of fluid we can make an estimate about how close a woman is to ovulation. The location of the dominant follicle can also tell us whether a woman is going to ovulate from the right or left ovary (which is helpful if one of the fallopian tubes is blocked or missing). If we see more than one large circle of fluid that often means more than one egg has developed.
If a woman is undergoing an IVF cycle her ovaries will have many of these large follicles, and this increased size of the ovaries is the reason for much of the bloating and discomfort of IVF. The process of ovulation is when the tiny egg bursts out of this circle of fluid and begins the journey into the fallopian tubes.
Ultrasound helps understand the woman’s cycle
During an IVF cycle the eggs are retrieved surgically by placing a very small tube with suction into each circle of fluid and draining out the fluid before ovulation has occurred. This fluid can then be examined under the microscope to find the mature eggs.
After ovulation this area on the ovary collapses and shrinks, often forming another collection of fluid known as a corpus luteum cyst. The timing of this collapse varies so it is challenging to tell by ultrasound exactly when ovulation has occurred. Performing ultrasound is what allows us to see where a woman is in the reproductive cycle, and whether she is responding to fertility medications to develop an egg or more than one egg. Hopefully if you understand what you are looking at those gray and black shadows from TVUS become a bit more interesting!
Blood tests make sure that hormone levels are okay during IVF
Our other method of understanding a woman’s response to treatment is by blood tests to check hormone levels. Those cells surrounding the egg that make fluid are also secreting a hormone called estrogen, so tracking the level of estrogen is another way we determine when the egg (or multiple eggs in an IVF cycle) are mature. There is no one number we are looking for when checking estrogen, as the appropriate value will depend on how many eggs are growing and how close she is to ovulation.
Performing blood draws as part of an IVF cycle is what allows your clinic to make sure you are responding safely, and sometimes adjust medication dosages up or down. Because an IVF cycle involves producing multiple eggs, it also means the estrogen level is much higher than in a cycle where only one egg grows. Many of the hormonal symptoms of IVF (headaches, moodiness or mood swings) are
related to this fluctuation of estrogen. I tell women not to be alarmed if they find themselves crying at commercials that normally would not affect them, or feeling irritable. Irritability during IVF is a very normal response to an unfair situation, and hormonal swings only magnify the situation.
Progesterone levels rise to support implantation
After a woman ovulates, the cyst that forms on the ovary begins to release a hormone called progesterone. This hormone is what helps to support implantation and early pregnancy. Women who have eggs surgically retrieved in IVF often require extra progesterone support (since the normal hormonal pathways and process of ovulation have been altered) and extra progesterone may be given post ovulation for other reasons as well.
Unfortunately, many symptoms associated with early pregnancy (breast tenderness, fatigue, constipation) are due to elevated progesterone levels, so women in fertility treatment on progesterone support should be careful to not overanalyze symptoms. Waiting until urine or blood tests can confirm the presence of hCG (the hormone made in early pregnancy) is the best way to know if pregnancy has occurred.
Treatment maximizes chances to conceive – but chances are limited
If you think too much about the many factors influencing conception, it can seem baffling and frustrating that so many get pregnant so easily. There are also many biological factors encouraging conception (such as chemical signals between egg and sperm) and likely many things we cannot yet test for or understand.
Treatments allow us to maximize our chances, but each month still provides only a limited chance of success, with an agonizing two week wait before knowing the cycle outcome. As much as it is helpful to read and understand the biology of reproduction, do not forget to check in and care for yourself emotionally.
Infertility hurts, be gentle with yourself
Infertility hurts. It hurts because of needles to check hormone levels or give medication. It hurts to undergo invasive testing or have a surgery. It also hurts to hear insensitive comments in the media or from friends and family. But mostly it hurts as a deep physical ache of wanting something and not knowing if it can happen, even if you try your very best.
Be gentle with yourself, realize you do have time. A month or two off can be the best treatment (and not because you’ll just get pregnant, as well wishing friends may suggest) but because you may need time to just be yourself and remember what it felt like when fertility wasn’t your whole life.
It will not always be your whole life, I promise. It is a chapter in it and your life will be different because of it, but it does not define you. I hope this article provides more understanding for your infertility journey, but information is only one piece. Your strength and core values define you, and once you get through infertility you can get through anything.



